Diabetes and Oral Health: A Connection You Should Not Ignore
Introduction
When people think about diabetes, they usually focus on blood sugar levels, diet, or medication. However, there is one area that is often overlooked — and that can have a direct impact on disease control: oral health.
The relationship between diabetes and oral health is reciprocal. On one hand, diabetes can increase the risk of oral problems. On the other hand, infections in the mouth, especially in the gums, can make it harder to control blood glucose levels.
Understanding this connection is essential to prevent complications and take care of overall health.
By Isabel Pais (Médica Dentista)
Edited by 2026-04-07
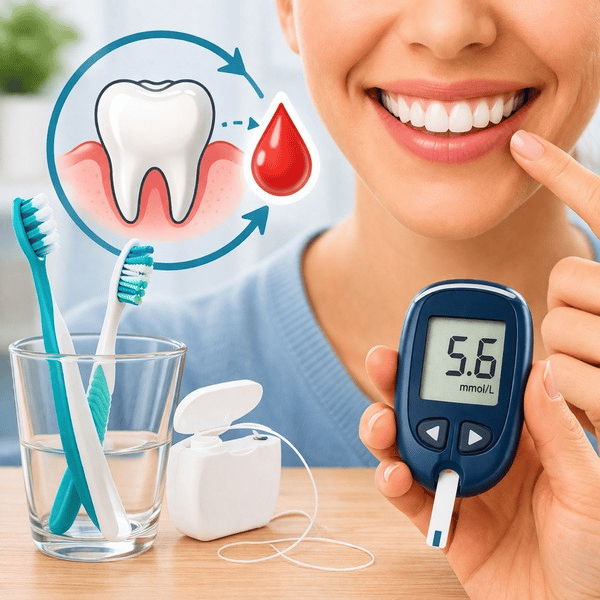
Diabetes and Oral Health: A Connection You Should Not Ignore
Introduction
When people think about diabetes, they usually focus on blood sugar levels, diet, or medication. However, there is one area that is often overlooked — and that can have a direct impact on disease control: oral health.
The relationship between diabetes and oral health is reciprocal. On one hand, diabetes can increase the risk of oral problems. On the other hand, infections in the mouth, especially in the gums, can make it harder to control blood glucose levels.
Understanding this connection is essential to prevent complications and take care of overall health.
By Isabel Pais (Médica Dentista)
Edited by 2026-04-07
How diabetes can affect oral health
When diabetes is not well controlled, the body reacts differently to infections and inflammation. This also happens in the mouth.
Gum problems (periodontal disease)
The gums are one of the most affected areas.
People with diabetes are at higher risk of developing:
- gingivitis (inflammation of the gums)
- periodontitis (inflammation of the supporting tissues of the teeth)
This happens because the body responds more intensely to the bacteria present in dental plaque, increasing inflammation and making healing more difficult.
Dry mouth
The sensation of dry mouth is more common in people with diabetes.
Saliva is essential because it helps to:
- clean the mouth
- control bacteria
- protect the teeth
When there is less saliva, the risk of cavities, infections, and oral discomfort increases.
Increased risk of infections
Diabetes can make the body more vulnerable to infections, including infections in the mouth.
One of the most common is oral candidiasis, a fungal infection that can cause:
- white patches
- burning sensation
- discomfort
Slower healing
Wounds or small lesions in the mouth may take longer to heal in people with diabetes, especially when blood sugar levels are high.
How oral health can affect diabetes
The relationship does not work in just one direction.
Chronic inflammation can interfere with the way the body uses insulin.
In practice, this may lead to:
- greater difficulty controlling blood glucose
- increased insulin resistance
- higher risk of diabetes complications
In other words, gum problems can make diabetes harder to control.
Can treating oral health help control diabetes?
Yes.
Studies show that treating periodontal disease may help improve blood sugar control.
It does not replace diabetes treatment, but it can be an important complement.
Warning signs
If you have diabetes, be alert to:
- red, swollen or bleeding gums
- persistent bad breath
- loose teeth
- frequent dry mouth
- pain or discomfort when chewing
The earlier these signs are identified, the easier it is to prevent complications.
What you can do daily
Small habits make a big difference:
- Brush your teeth at least twice a day
- Use dental floss daily
- Visit your dentist regularly
- Maintain good blood glucose control
- Avoid smoking
Oral health should be part of the routine of people living with diabetes.
A holistic approach to health
Today we know that health should not be viewed in isolation.
The mouth is not separate from the rest of the body — and diabetes is a clear example of this.
Taking care of your gums and teeth is not just about aesthetics.
It is a way to protect overall health and improve disease control.
Conclusion
The connection between diabetes and oral health is real and has a daily impact.
Controlling diabetes helps protect the mouth.
Taking care of the mouth helps control diabetes.
This balance is essential to prevent complications and improve quality of life.
Sources
This article is based on recommendations and scientific evidence from international organizations such as the World Health Organization (WHO), International Diabetes Federation (IDF), American Diabetes Association (ADA), Centers for Disease Control and Prevention (CDC), National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), and the joint consensus of the European Federation of Periodontology (EFP) and IDF, as well as scientific literature published in journals such as Journal of Clinical Periodontology, Diabetes Care, and Journal of Periodontology.